Check the Neck after a Brain Injury
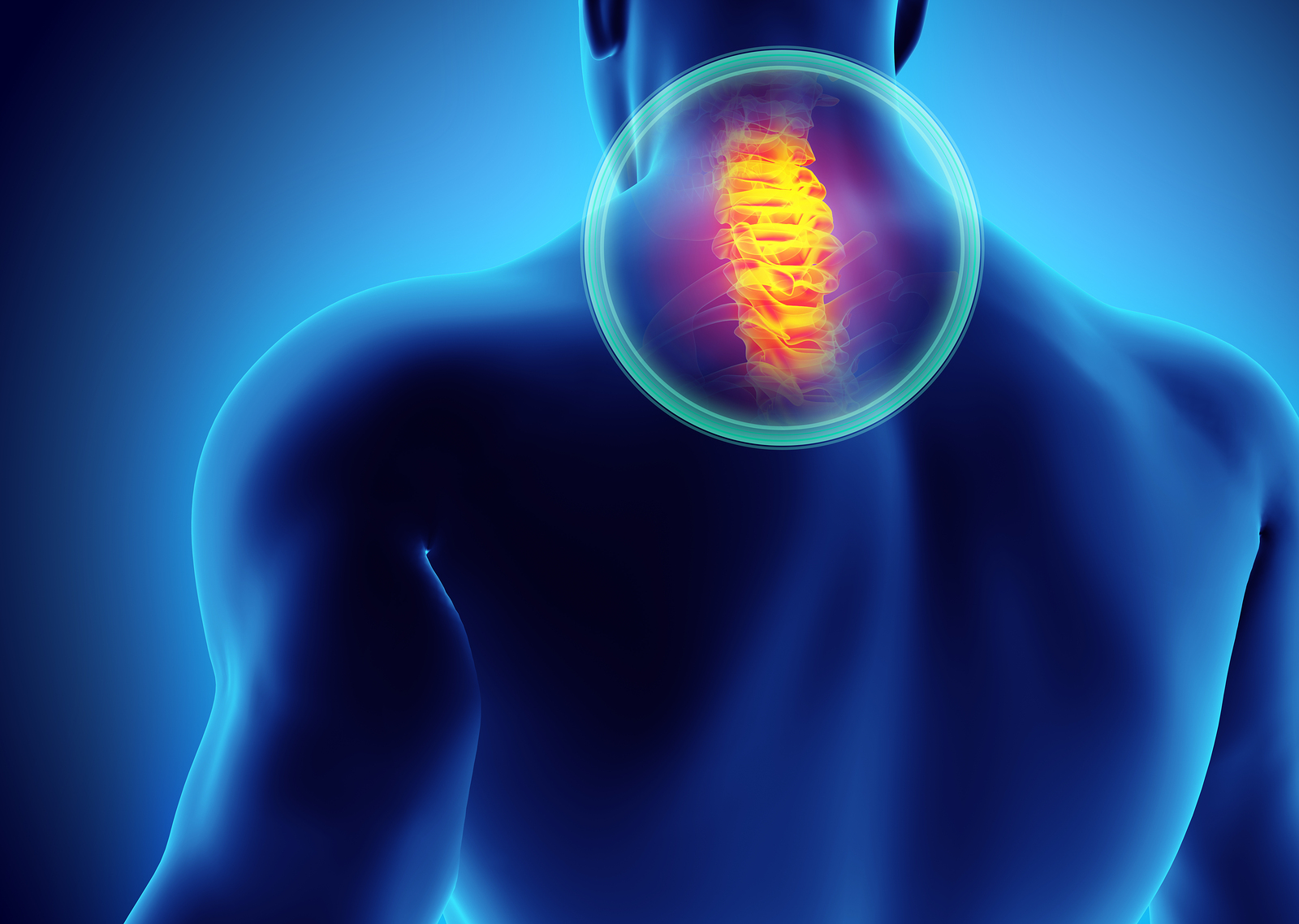
Whiplash occurs when the head and neck are suddenly forced back and then forward (or forward and then back), producing large amounts of stress on the soft tissues of the neck. Whiplash and cervical strain both refer to damage of the muscles, ligaments, or tendons in the neck.
While whiplash is most commonly associated with car accidents, it can also occur in sports injuries, cases of assault, and slips and falls, to name just a few examples. It’s so common in people who have a concussion or TBI because the average amount of force causing a concussion – about 95 g’s – is much, much higher than the force required to injure the neck – as little as 5 g’s. Therefore, the majority of people who suffer a concussion or TBI will also experience neck injury.
Symptoms of whiplash and cervical strain are very similar to symptoms of concussion, and include:
- Headache
- Neck pain, tightness, or tenderness
- Reduced range of motion in the neck
- Dizziness
- Ringing in the ears
- Fatigue
- Blurred vision
- Nausea or vomiting
Symptoms often appear soon after the injury but sometimes arise only after a few days.
To diagnose whiplash, your doctor will examine you and ask for your history and may also use imaging techniques. Standard x-rays may be used to rule out other causes of neck pain, but can’t show damage to the soft tissues. MRI and CT may be used to see more parts of the anatomy like the cervical discs, vertebral joints, or soft tissues.
Treating whiplash and cervical strain in TBI cases
Luckily, whiplash injuries usually heal within a short period of time and without much intervention. Ice to the neck, a neck brace, and painkillers are common short-term treatments. You should always speak with your doctor before starting any kind of treatment plan. Remember that soon after a concussion or brain injury you should not treat your pain with aspirin or anti-inflammatory medicines like ibuprofen due to an increased risk of bleeding until your doctor says it is OK.
For chronic whiplash pain, additional treatment may be pursued, such as physical therapy, chiropractic care, or injections. Improving posture and increasing strength and flexibility in the neck are also helpful in resolving the condition.
Learn more about brain injury and rehabilitation
Check out other places on my website where I discuss headaches and neck pain:
You Might Also Like
Managing Concussion-Related Pain
Dr. Steven Moskowitz is a physiatrist specializing in pain management. He discusses the various painful conditions, including neck pain and headaches, that occur at high frequency after concussion and related trauma. He advocates for a biopsychosocial approach to the evaluation and treatment of these conditions.
3 Things to Do to Allow Your Brain to Recover More Quickly After Brain Injury
After a concussion, people need good sleep patterns, and they also need to resume activity and exercise to aid recovery. Activities with concussion risk should be avoided, however.
Keep up to date
Get updates on the latest in concussion, brain health, and science-related tools from Dr. Elizabeth Sandel, M.D.
By clicking SIGN UP, you agree to receive emails from Dr. Sandel and agree to our terms of use and privacy policy.
Get the book!



