Archive
Diagnostics
Learn about diagnostic evaluations of concussions and other brain injuries.
Check the Neck after a Brain Injury
Whiplash and cervical strain occurs when a person’s head and neck are forced back and forth, injuring soft tissues of the neck. They are common after brain injuries.
Evaluating and Treating Headaches After Brain Injury
Headaches are extremely common after a traumatic brain injury, but there are various treatments that vary depending on the phenotype or cause.
Post-Traumatic Headaches: Not Just One Type or Treatment
Headaches must be evaluated with a comprehensive history and physical examination. There are many options for treatment, but diagnosis has to be the first step.
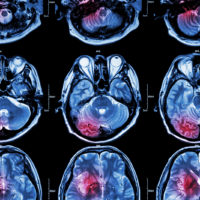
Brain Imaging after an Injury
CT and MRI scans are the most common imaging modalities to evaluate people with traumatic brain injury, but advanced imaging methods are more promising for diagnosis and prognosis. However, interpretations of findings can vary.
Why is “Post-Concussion Syndrome” Controversial?
We do not yet have a clear understanding of what happens in the brain immediately after a concussion and over the days and months that follow, especially for those patients whose symptoms persist. Post-concussion symptom rates vary greatly among research studies, likely because the populations studied are diverse and so are the diagnostic criteria and timing of assessments. The wide variation in symptom rates highlights the fact that there is a lot we still don’t know about concussions.
Top Causes of Concussion in Children and Adolescents
When we think of “youth” and “concussion,” the first thing that likely comes to mind is a teenager engaging in a high-risk activity such as football, soccer, or snowboarding. But not all youth brain injury results from these risky activities. Of the millions of concussions reported by emergency rooms every year, figures put concussions related to sports and recreation at just 30% – so 70% of concussions result from other causes.
Is Concussion a Diagnosis?
Clinicians like me say that concussion requires a clinical diagnosis based on the history of what happened to produce the symptoms. However, because these same symptoms appear in other conditions, and we don’t have reliable biomarkers, diagnosing a concussion can sometimes be a challenge. The lingering effects of a mild brain injury can also continue as a chronic condition, often referred to as post-concussion syndrome or persistent post-concussion symptoms, that still require treatment.
Mood Disorders Such as Depression Can Complicate a Brain Injury
A traumatic brain injury can be associated with depression or another mood disorder, possibly because of the disruption of brain chemicals.
A Patient-Centered Approach to Concussion Care: CME & Webinar
Elizabeth Sandel, MD, a physiatrist and brain injury medicine physician, and Conor Gormally, co-founder of Concussion Alliance — a young man who has experienced several concussions — present a patient-centered care approach for emergency medicine and primary care physicians.
Will My Child Experience Long-Term Consequences from a Concussion or other Brain Injury?
Although most children recover fully after a single concussion, others have long-term effects. Of course, prevention is the best strategy, but if a concussion occurs, parents must understand a brain injury has occurred.
How Long Will It Take for My Child to Recover from a Concussion?
Children can experience a range of symptoms after concussion. They require individualized treatments and strategies for returning to activities and to school. A physician with training and experience in treating concussions must provide early interventions and follow-up, regardless of how long recovery takes.
Self-Reported Concussion Symptoms are Key to Evaluation & Diagnosis
To properly diagnose a concussion and devise a treatment plan requires a thorough physician evaluation, a symptom checklist or an interview, or both, followed by a comprehensive cognitive and physical examination. Download a pocket guide that helps patients prepare for being evaluated.
Keep up to date
Get updates on the latest in concussion, brain health, and science-related tools from Dr. Elizabeth Sandel, M.D.
By clicking SIGN UP, you agree to receive emails from Dr. Sandel and agree to our terms of use and privacy policy.