How Long Will It Take for My Child to Recover from a Concussion?
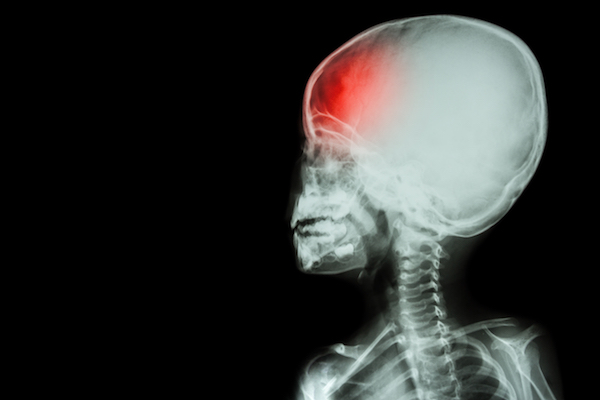
A concussion (a mild traumatic brain injury) occurs when a sudden force on the head or body causes the brain to move inside the skull, injuring it. Falls, sports, recreational injuries, motor vehicle accidents, and assaults, often from child abuse, can all cause concussions in children. A significant proportion of concussions are sports-related.
It’s not usually possible to see any damage that a concussion has done to the brain with imaging studies or even a physical examination. The term “mild” in “mild traumatic brain injury” – another term for a concussion – refers to the fact that loss of consciousness is at most brief, or the period of amnesia (memory loss) or confusion is relatively short compared with more severe injuries. It doesn’t mean that the injury itself, or its consequences, are “mild.” The diagnosis is made without a definitive “biomarker” – a laboratory or imaging study.
Initial Symptoms of Concussion
Common symptoms that appear soon after the concussion was sustained include:
- Headaches
- Blurred vision
- Sensitivity to light
- Dizziness
- Loss of balance
- Fatigue
- Sleep disturbances
- Memory problems (remembering old information, making new memories)
- Confusion
- Poor concentration
- Learning problems
- Mood swings and irritability
- Depression
I developed a pocket guide for adults and family members of children with concussions that gives more information about “red flag” symptoms and how to prepare for a visit with your physician.
Recovery from a Concussion: What to Expect?
If your child has suffered a concussion and is experiencing symptoms, you may be wondering how long it will be before those symptoms lessen and eventually resolve. The good news is that concussion symptoms typically go away in most children within the first month after injury, at least after a first concussion. The bad news is that approximately one in every three or one in every four children with a concussion may continue to have persistent symptoms beyond a month. If children do not recover, they will likely experience physical, cognitive, or emotional symptoms that affect functioning and quality of life.
Chronic symptoms can persist for many months or, rarely, for years after a concussion. These symptoms can interfere with your child’s academic and social life. Sensitivity to light and sounds can make it difficult for your child to tolerate being in the classroom. Memory and focus problems make it hard to concentrate in class and get homework done. Irritability and moodiness can cost friendships and cause difficulties in school or at home.
Persistent Post-Concussion Symptoms
Symptoms of a chronic and persistent condition after a concussion have been called “post-concussion syndrome,” but this is not a syndrome with a definite set of symptoms. I prefer the term “persistent post-concussion symptoms.” Your daughter or son may continue, for example, to have headaches and problems with learning new information, but perhaps not dizziness or balance problems. Or maybe your child will have mood swings and difficulty sleeping after a concussion, but no headaches.
Research tells us that children are more likely than adults to develop persistent post-concussive symptoms, and younger children are more likely than older children to develop it. Other factors associated with an increased likelihood of a more chronic or ongoing condition are a history of repeated concussions, learning disabilities, attention deficit hyperactivity disorder (ADHD), and depression and anxiety. Read more about these conditions and their relationship to concussions in another post here.
Risk Scoring for a Child’s Concussion?
Dr. Roger Zemek of Children’s Hospital of Eastern Ontario, and the University of Ottawa, Canada, and his colleagues conducted a study to derive and validate a clinical risk score to stratify “persistent postconcussive symptom (PPCS) risk” after acute concussion in children and adolescents (age 5-<18 years) who arrived within 48 hours to a pediatric emergency department, with follow-up at 28 days after the injury. The study’s primary outcome was the risk score at 28 days, defined as three or more new or worsening symptoms. The risk score incorporates clinical variables related to demographics (age and sex), history, initial symptoms, cognitive complaints, and a physical examination.
In this Canadian study, persistent symptoms were present in 31 % of the children at 28 days. Certain risk factors suggested a higher probability of continuing symptoms: female sex, age of 13 years or older, migraine history, prior concussion with symptoms lasting longer than one week, headache, sensitivity to noise, fatigue, answering questions slowly, and errors on a balance test. Dr. Zemek and his colleagues offer professionals excellent concussion tools and guidelines for assessing risk and providing concussion care on their website.
Dr. John Leddy and his colleagues at the University of Buffalo have also identified some symptoms and physical examination findings that appear to be risk factors.
What You Can Do as a Parent
The key is to communicate with your physician and other healthcare professionals about the need for ongoing evaluations and treatment. Share the information from this post with your child’s primary care physician.
Keep track of your child’s recovery, and report any new symptoms you notice. You can speak with their teachers and school administrators to ensure they get educational support and accommodations under Section 504 of the Rehabilitation Act. If the concussion was sports-related, talk to your child’s coaches to ensure that protocols are in place to help prevent and recognize concussions in all children who are at risk.
Learn More About Children and Concussion
There’s a lot to talk about regarding children and concussions. You can find other information in my book, Shaken Brain, and in other blogs and interviews on this website.
You Might Also Like
Be a Parent Advocate for Children and Youth Sports Concussions
Parents must communicate with the school after their son or daughter has a concussion to make sure that there are accommodations if needed during recovery.
Concussions in Young Children
Dr. Maya Evans is a pediatric physiatrist who treats children and adolescents with brain injuries, including concussions. She discusses the special needs of these populations for expert care and also advocates for prevention strategies.
A Parent’s Key Role after a Child’s Concussion
Parents play a major role in identifying the effects of concussions in their daughters and sons, helping them manage symptoms, and supporting their recovery.
Concussion in Young Children: What You Need to Know
An early childhood teacher talks with Dr. Sandel about about concussion in young children. What causes it? What do we need to look for? And how can we help during the recovery process?
Parents and Sports-Related Concussions
Michelle Camicia, MSN, PhD, the mother of two student athletes, discusses the role of parents who must pay attention to their childrens’ symptoms if they play contact sports. Are these symptoms consistently understood by student athletes and coaches? She argues for more education and advocacy to address the problem of…
Nurse Rona Interviews Dr. Elizabeth Sandel
Nurse Rona Renner of KPFA interviews Dr. Sandel about her book, Shaken Brain. They discuss the many causes of concussions and how patients are best evaluated and treated. She fields questions about the neurodegenerative conditions that are associated with brain injuries, especially repetitive brain injuries.
Keep up to date
Get updates on the latest in concussion, brain health, and science-related tools from Dr. Elizabeth Sandel, M.D.
By clicking SIGN UP, you agree to receive emails from Dr. Sandel and agree to our terms of use and privacy policy.
Get the book!