Repetitive Brain Trauma and Chronic Traumatic Encephalopathy (CTE)
Research Links CTE to American Football & Other Collision Sports
On April 7, 2021, Phillip Adams, a 32-year-old NFL player who played for six teams over two decades, killed six people including two children, and then shot himself with the same gun on in a North Carolina town. Those killed were a prominent local physician, his wife and their two grandchildren, and two men working at the home where the murders took place. Adams died of a self-inflicted gunshot wound. His family made a donation of his brain to Boston University’s brain bank to find some answers to explain this horrific saga.
Boston University pathologist Ann McKee’s confirmed that Adams had chronic traumatic encephalopathy (CTE), a neurodegenerative disease clearly linked to American football, and most likely other collision sports where repetitive brain trauma occurs. The first cases of the disease were in described in boxers in the 1920s.
Stages of Trauma-Induced Neurodegenerative Brain Disease
Dr. McKee’s laboratory has now analyzed hundreds of brains from legacy donors and developed a staging system for CTE that has now been validated. Researchers are uncovering the clear link between repetitive brain injuries and CTE. Under the microscope they can see how tau, a protein in the microtubules of axons (the scaffolding of the neuron’s connecting tracts), changes to phosphorylated, “p-tau” and then becomes distorted into neurofibrillary tangles. This happens especially in the neurons occupying the sulci (crevices or valleys) of the brain, progressing through four stages to affect the entire brain. Inflammation and breakdown of the blood-brain barrier also drives more destruction of brain tissue, and the disease is, by definition, progressive.
In my book, Shaken Brain: The Science, Care, and Treatment of Concussion, I discuss these microscopic processes in more detail. Read Chapter 4 (Late Effects) for more about the science related to CTE and other neurodegenerative diseases linked to brain injury. I also share an earlier case from Dr. McKee’s brain bank case series in my book: New England Patriot player Aaron Hernandez. Hernandez was convicted of murder and died in prison of suicide in 2015 at the age of 27. He had Stage 3 CTE which is represented in an illustration from my book here:
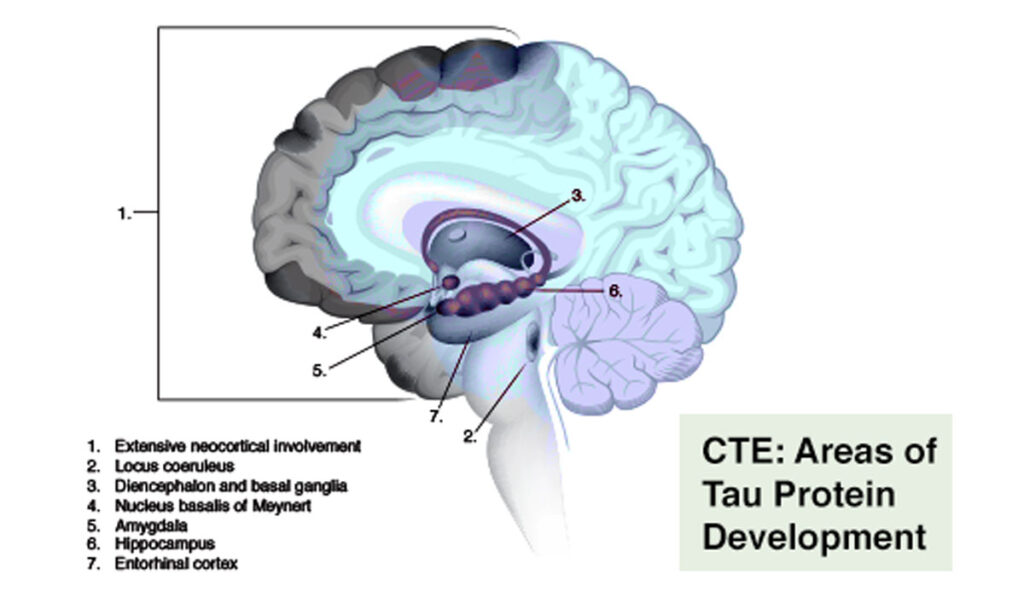
CTE Risk Factors
Dr. McKee and colleagues, including Michael Alosco, Jesse Mez, Julie Stamm, Robert Stern, and others have researched the risk factors for CTE. They discovered that the disease can result from repeated concussions but more likely results in many “subconcussions” or “hits” where the impact or “g” forces aren’t great enough to produce symptoms but are doing damage to the brain nevertheless. The number of seasons played as well as the age of “first exposure” to football (especially if played before age 12) heightens the risk of CTE. The odds for getting CTE appear to double for every 2.6 years of football played, and players with 11 or more years of tackle football carry a significant risk. CTE does not seem to occur without this repetitive brain trauma. However, not everyone who plays football gets CTE. Genetics, gender, race-ethnicity, social determinants of health may play a role in risks for CTE, but more research needs to be done to establish their relationship, if any, to CTE.
Causes of repetitive brain injury other than American football are likely risk factors, too. These causes include other contact and collision sports — for example, soccer, rugby, hockey, lacrosse, wrestling, and cheerleading. Military service, intimate partner violence, and certain occupational categories such as jockeys or first responders may also carry a risk of CTE. Unfortunately, research into these populations is scant compared with American football.
CTE Diagnosis
There is now an attempt to diagnose CTE before death using clinical criteria for what is termed traumatic encephalopathy syndrome (TES). TES is the clinical term for people who likely have CTE. The disorder is marked by changes in emotional control with violent and explosive behavior, cognitive deficits, Parkinson-like symptoms and signs, gait disturbance, and dysarthria (difficulty speaking clearly), and dementia. Eventually laboratory biomarkers and advanced neuroimaging studies will become clinically available to diagnose CTE.
CTE Treatment
There is little if any research regarding successful treatments for TES. Neurologists, physiatrists, and psychiatrists can help to determine what medications could ameliorate symptoms and improve quality of life for people with CTE. Medications for Alzheimer’s Disease or Parkinson’s Disease, for mood disorders such as anxiety and depression, and for chronic pain may be helpful. The benefits of good nutrition, promotion of good sleep-wake cycles, and aerobic exercise may be very beneficial. Neuropsychological evaluations are informative for understanding cognitive and psychological functioning and for identifying treatment strategies. Mental health services and rehabilitation treatments such as those provided by physical, occupational, and speech therapists can be very valuable, especially when delivered with a team-based approach.
Learn More about Trauma-Induced Neurodegenerative Brain Disease
I am a member of an international group, The Repercussions Group, whose mission is “…to insist upon ethical and transparent research into trauma-induced brain injury from a person-centred perspective and for that research is warranted to subsequently inform the prevention, diagnosis and treatment and outcomes of trauma-induced neurodegenerative brain disease.” If you want to know more about the Group’s work, view the YouTube video here:
Medical historian Stephen Casper of Clarkson University led the effort with members of The Repercussions Group to publish an article critiquing the International Consensus Statements on Concussion in Sports that have been published since 2001. The 5th was published in 2016 and the 6th is due out in the summer of 2022. We argue that:
“there is a strong need for a new approach to them that foregrounds public health expertise and patient-centered guidance. Doing so will help players, parents and practitioners keep perspective about these potentially life-altering injuries especially when they recur.”
Casper, S., Bachynski, K., Buckland, M., Comrie, D., Gandy, S., Gates, J., . . . Finkel, A. (2021). Toward Complete, Candid, and Unbiased International Consensus Statements on Concussion in Sport. Journal of Law, Medicine & Ethics, 49(3), 372-377. doi:10.1017/jme.2021.56
If you want to read more about the lives of people who have suffered from CTE and their families, I recommend these two books:
You Might Also Like
The Prevalence of Brain Injuries in Sports and the Military
In the second part of this series, Dr. Sandel continues with further discussion of concussion management. She then describes blast injuries that occur in the military. Who provides treatment for concussions and what kind of care is best?, What are the risks of a long-term problem after a concussion or…
The “Invisible Injury”: Concussions and other TBI’s
In the first part of this series, Dr. Sandel discusses mild brain injuries, especially sports-related concussions. What happens to the brain during a concussion and what are the symptoms? What is second impact syndrome? And are children more or less vulnerable than adults?
Nurse Rona Interviews Dr. Elizabeth Sandel
Nurse Rona Renner of KPFA interviews Dr. Sandel about her book, Shaken Brain. They discuss the many causes of concussions and how patients are best evaluated and treated. She fields questions about the neurodegenerative conditions that are associated with brain injuries, especially repetitive brain injuries.
Keep up to date
Get updates on the latest in concussion, brain health, and science-related tools from Dr. Elizabeth Sandel, M.D.
By clicking SIGN UP, you agree to receive emails from Dr. Sandel and agree to our terms of use and privacy policy.
Get the book!




