Traumatic Brain Injury and the Elderly

Head Trauma is a Leading Cause of Decline and Death for Older Adults
Traumatic brain injury (TBI) is a leading cause of morbidity and mortality among the elderly. Older adults with TBIs are more likely to die or require long-term care than younger people. Chronic health conditions make older adults more susceptible to falls, the most common cause of these injuries. They commonly take more medications in general and more medications that can cause balance problems, falls, and confusion or that lead to more bleeding in the brain. Most of the falls in the elderly are ground-level falls, not falls from heights.
The second most common cause of traumatic injury is motor vehicle collisions. While these cases are less common than falls, motor vehicle collisions are more likely to cause mortality in older patients.
Elder Abuse: A Hidden Cause of TBI
In my book, Shaken Brain (Chapter 8), I discuss another cause of TBIs in older adults – elder abuse. Abuse can be an unrecognized cause of a TBI in an older person and can be physical, psychological or verbal, sexual, or financial. Neglect is also a type of elder abuse that may also lead to traumatic injuries.
Elder abuse is on the rise, and estimates are that one in ten seniors experiences some form of elder abuse every month. Because many abuse cases go unreported, this is likely an underestimate. Those at highest risk are the “young old” – those more likely to live with a spouse or adult children (the most common abusers). Older people with dementia and those with lower socioeconomic status are at higher risk. Abusers are more likely to be male and to have a mental health condition or a history of substance abuse.
The higher incidence of chronic dementia in the elderly may cause delays in the presentation and treatment of TBI. Obtaining an accurate history and physical exam in an elderly patient with dementia can be challenging. A TBI, especially if severe, may render an older adult unconscious or cloud their memory of what actually happened. The history might be obtained from family, friends, bystanders, or emergency personnel, but this information may be missing or covered up in elder abuse or elder neglect circumstances.
Anatomic Differences Make the Elderly More Susceptible to TBI
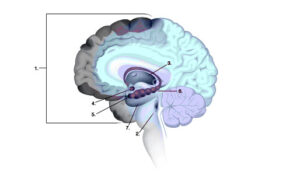
Anatomic differences make older adults more susceptible to bleeding in the brain from blunt head trauma or inertial injuries. There is increased adherence of the dura (a membrane covering the brain) to the skull, and brain atrophy and stretching of the bridging veins can lead to more damage in older people. Delays in diagnosis and treatment contribute to higher morbidity and mortality in the elderly. (See my book, Shaken Brain, for more information and illustrations on this topic.)
Various medical conditions require anticoagulation, including atrial fibrillation, pulmonary embolism, or deep vein thrombosis. Coumadin (warfarin) has been the most commonly used anticoagulant, but newer anticoagulant medications are frequently prescribed. These medications increase the amount and rate of bleeding in the brain, thus increasing the risk of death or severe disability due to a TBI.
Bruising may be the only indication of a traumatic injury. The history and physical examination may be unreliable for many reasons. Acute neurological findings may be challenging to differentiate from chronic findings. Finally, a stroke may result in signs and symptoms similar to a TBI.
Prevention of TBI in the Elderly
Strategies to prevent TBIs in the elderly include fall prevention and crucial patient and caregiver education. Ambulation assistance devices such as canes, walkers, and eventually scooters or wheelchairs can help prevent falls. Physicians must assess older patients for seizures and syncopal episodes and medical conditions which are causing impaired vision, weakness, and balance problems. These assessments may suggest that an elderly patient cannot safely operate a motor vehicle. If indicated, physicians must report this information to the State’s department of motor vehicles to conduct further evaluations.
Physicians and clinical teams in inpatient and outpatient settings must work with the patient, family, and friends to provide TBI resources and prevention strategies. Social workers, nurses, and spiritual and palliative care professionals can be essential members of these teams. For patients who might require anticoagulation, the physician should initiate a thorough discussion of the risks and benefits of anticoagulation so that the patient and family can make an informed decision.
Report Elder Abuse
For elders with injuries from suspected elder abuse, those responsible for reporting (mandated reporters) must follow their State’s legal requirements. If someone you know is in immediate and life-threatening danger, call 911. For other cases of suspected abuse, call the Eldercare Locator at 1-800-677-1116 for information about local agencies.
You Might Also Like
Falls and Brain Injury in Older Adults
Traumatic brain injuries are very common in older adults who fall. They can result in hospitalization, death, or disability especially in this age group and those on certain medications. In this post, an elderly woman has a delayed hematoma from an injury that could have been deadly. Falls can be prevented and Dr. Sandel shares important information about risk factors and tips for prevention.
Repetitive Brain Trauma and Chronic Traumatic Encephalopathy (CTE)
There’s a link between chronic traumatic encephalopathy (CTE) and repetitive brain injuries that occur in boxing and American football. This is a progressive neurodegenerative disorder that can lead to severely-disabling neurologic and psychiatric disorders. Learn about the science, diagnostic criteria for traumatic encephalopathy syndrome (TES), and possible treatment approaches.
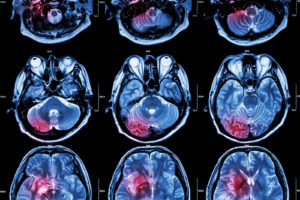
Brain Imaging after an Injury
CT and MRI scans are the most common imaging modalities to evaluate people with traumatic brain injury, but advanced imaging methods are more promising for diagnosis and prognosis. However, interpretations of findings can vary.
Keep up to date
Get updates on the latest in concussion, brain health, and science-related tools from Dr. Elizabeth Sandel, M.D.
By clicking SIGN UP, you agree to receive emails from Dr. Sandel and agree to our terms of use and privacy policy.
Get the book!