Archive
Conditions
Traumatic brain injuries may lead to a number of conditions, such as persistent post-concussion syndrome, disorders of consciousness, or neurodegenerative diseases.
Is There a Connection Between Mild TBI and Mental Health Disorders in Adults and Children?
In a recent study, researchers at Kaiser Permanente found that risks for affective and behavioral disorders were significantly higher in the years post-injury for children and adolescents with a history of mTBI—especially for 10- to 13-year-olds. They emphasize the importance of regular interval screening for affective and behavioral disorders in children and adolescents who sustain a mild TBI. This post includes a slide presentation and Q & A with two of the researchers, Richard Delmonico, PhD, and Brian Theodore, PhD.
Why I Am Not Surprised About the Latest CTE Research
Millions of children play contact and collision sports in the US, with high risks for head impacts. Repetitive hits can result in concussions or subconcussions without immediate evidence of neurologic injury. CTE is a brain disorder caused by repetitive hits to the brain from sports such as football and soccer. The latest study from Dr. Ann McKee’s brain lab at Boston University links CTE to child athletes who died before the age of 30.
Treatment and Prognosis after a Concussion
Learn about treatments for post-concussion symptoms—including medication, various rehabilitation therapies, neuropsychology, and potentially some complementary therapies—as well as factors related to longer concussion recovery times.
Patient and Provider Perspectives on Improving Care for Post-Concussion Symptoms
This poster, created for the International Brain Injury Conference in New York in Sept 2022, offers various perspectives on how to improve concussion care. Attached are a reformatted poster presentation and related webinar links.
Why is “Post-Concussion Syndrome” Controversial?
We do not yet have a clear understanding of what happens in the brain immediately after a concussion and over the days and months that follow, especially for those patients whose symptoms persist. Post-concussion symptom rates vary greatly among research studies, likely because the populations studied are diverse and so are the diagnostic criteria and timing of assessments. The wide variation in symptom rates highlights the fact that there is a lot we still don’t know about concussions.
Is Concussion a Diagnosis?
Clinicians like me say that concussion requires a clinical diagnosis based on the history of what happened to produce the symptoms. However, because these same symptoms appear in other conditions, and we don’t have reliable biomarkers, diagnosing a concussion can sometimes be a challenge. The lingering effects of a mild brain injury can also continue as a chronic condition, often referred to as post-concussion syndrome or persistent post-concussion symptoms, that still require treatment.
Mood Disorders Such as Depression Can Complicate a Brain Injury
A traumatic brain injury can be associated with depression or another mood disorder, possibly because of the disruption of brain chemicals.
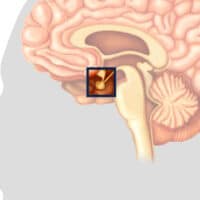
How Does Brain Trauma Affect Brain Hormones?
Evaluating and treating people with hormonal deficiencies after traumatic brain injury (TBI) can be very challenging. Learn about the screening and treatment of pituitary deficiencies that may occur in both the acute and chronic stages after a concussion or other TBI.
Opioids Cause Problems After a Brain Injury
Stories of opioid-related disability and death are in the news frequently because of a surge in the use of these substances over the past few decades. For people with a history of brain injury, including concussions, the risks of using opioids are higher than for those without this medical history. Learn about the benefits and dangers of these substances, some of which are not only legal but widely prescribed for acute and chronic pain.
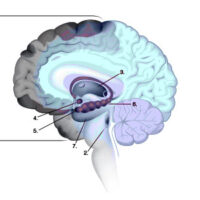
Coma and Other Disorders of Consciousness
What happens to the brain after a severe brain injury that renders a person unconscious or “comatose”? Learn the meaning of other terms that describe patients who have disorders of consciousness: the minimally conscious state, cognitive-motor dissociation, covert consciousness, and unresponsive wakefulness syndrome (vegetative state). Researchers are studying advanced technologies evaluating patients with disorders of consciousness, and there are new U.S. and European guidelines that are helping to standardize care and advance the field of brain injury.
Repetitive Brain Trauma and Chronic Traumatic Encephalopathy (CTE)
There’s a link between chronic traumatic encephalopathy (CTE) and repetitive brain injuries that occur in boxing and American football. This is a progressive neurodegenerative disorder that can lead to severely-disabling neurologic and psychiatric disorders. Learn about the science, diagnostic criteria for traumatic encephalopathy syndrome (TES), and possible treatment approaches.
What is Post-Concussion Syndrome?
I recently talked with journalist Nathaniel Parish Flannery who writes about cycling. He was writing an article about pro cyclist Ian Boswell. Boswell had a crash in 2019 that resulted in long-term concussion symptoms. Flannery found our conversation and my book, Shaken Brain, very helpful, and he tells Boswell’s story in…
Keep up to date
Get updates on the latest in concussion, brain health, and science-related tools from Dr. Elizabeth Sandel, M.D.
By clicking SIGN UP, you agree to receive emails from Dr. Sandel and agree to our terms of use and privacy policy.